Glaucoma
What is Glaucoma?
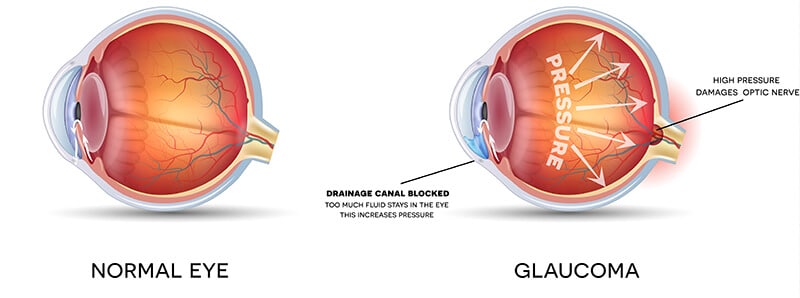
Glaucoma is one of the leading causes of blindness and visual impairment in the United States and can affect patients of all ages, many of who do not experience any symptoms and may not be aware that they have the disease. Glaucoma actually refers to a group of diseases that cause damage to the optic nerve, usually as a result of increased pressure within the eye. Glaucoma is usually painless and produces no symptoms until significant vision loss has occurred.
There are two main types of glaucoma, angle-closure and open-angle. Angle-closure glaucoma involves a sudden buildup of pressure in the eye and poor drainage because the angle between the iris and the cornea is too narrow. Open-angle glaucoma is the most common type of glaucoma and involves fluid in the eye not draining properly from inside the eye.
Angle-closure glaucoma
Angle-closure glaucoma can develop after many years without causing pain or other noticeable symptoms, so you may not experience vision loss until the disease has progressed. This makes it difficult for many patients to know if they have glaucoma. As glaucoma progresses, patients may experience a loss of peripheral or side vision, along with sudden eye pain, headache, blurred vision or the appearance of halos around lights. This is considered an emergency and patients must seek medical attention immediately to prevent blindness.
If Dr. Stancey determines you have narrow-angles or angle-closure, they may recommend a laser procedure to reduce your risk of glaucomatous vision loss. If you have cataracts, surgery to remove them may also be recommended as this increases the space inside the eye to open the angle. Click here to read more about cataract surgery.
Risk factors for angle-closure glaucoma include:
- Asian or Indian descent
- Female
- Being far-sighted (hyperopic)
- Family history of narrow-angles or angle-closure
Open-angle glaucoma
Open-angle glaucoma occurs in 90% of glaucoma patients and is thought to be due to a diseased drainage system called the trabecular meshwork. While some patients may experience symptoms from glaucoma as the disease progresses, others do not learn they have the condition until they undergo a routine eye exam. There are several different exams performed to diagnose glaucoma, including a visual field test to check peripheral vision and an OCT (optical coherence tomography) to access the health of the optic nerve fibers. Tonometry is performed to measure the pressure inside the eye. Other tests may also be performed, such as pachymetry to measure the thickness of the cornea, which influences the measurement of the true pressure in the eye, and gonioscopy, which uses a lens to visualize the angle and trabecular meshwork.
Once glaucoma has been diagnosed, treatment should begin as soon as possible to help minimize the risk of permanent vision loss. While doctors used to treat glaucoma only when there was vision loss, we now try to treat patients before vision loss occurs. There is no cure for glaucoma, so treatment focuses on relieving symptoms and preventing further damage. Most cases of glaucoma can be treated with eye drops to help lower the eye pressure. Sometimes, laser or surgery is recommended. The best treatment for your individual case depends on the type and severity of the disease, and can be discussed with Dr. Stancey.
Common risk factors for open-angle glaucoma include:
- Over the age of 60
- African Americans over the age of 40
- Trauma
- Diabetes
- Being near-sighted (myopic)
- Family history of glaucoma
- Steroid use – oral, inhaled, injected, or over-the-counter nasal sprays
In the past, ophthalmologists believed that glaucoma could only occur when the intraocular pressure (IOP) was >21 mmHg. However, we now know that glaucoma can occur even in patients with seemingly normal IOP. These patients have what’s called normal tension glaucoma, which is a form of open-angle glaucoma. There is some thought that low blood pressure especially at night or dysregulation of the vascular (blood system) is to blame.
Other types of glaucoma include congenital glaucoma, which develops in newborns due to an abnormal drainage system, pigmentary glaucoma, which results from increased pigment cells that block the drainage system, pseudoexfoliation glaucoma, which results from a protein-like material that blocks the drainage system, neovascular glaucoma due to systemic issues like diabetes or ocular issues such as vein occlusion, and traumatic glaucoma which results from physical trauma to the eye, among many other types.
You may be diagnosed as a glaucoma suspect if your optic nerve appears suspicious for glaucoma but does not yet meet criteria for glaucoma. Glaucoma suspects should have a comprehensive dilated exam with necessary testing at least every year to ensure it hasn’t progressed to glaucoma.
Excellent information can be found at:
The Glaucoma Research Foundation
The American Academy of Ophthalmology
The International Glaucoma Association